
- 198 pages
- English
- ePUB (mobile friendly)
- Available on iOS & Android
eBook - ePub
About this book
Despite the various advantages of home dialysis compared to in-center hemodialysis, only a fraction of patients in Japan currently opt for peritoneal dialysis or home hemodialysis. However, considerable advances in research and technical improvements have been made lately, advancing the practice of home dialysis therapy in Japan. Japanese research is well-known for its ingenuity and creative energy with regard to the development of new machines and systems for dialysis. New insights regarding peritoneal dialysis and home hemodialysis are presented in the publication at hand: Contributions by leading Japanese experts discuss topics such as educational methods, techniques, tools, novel systems and organization of patients. The book will be of great interest to clinical physicians involved in dialysis care; Moreover, the expertise collected in this volume may contribute to the advancement of home dialysis therapy in a global context.
Trusted by 375,005 students
Access to over 1.5 million titles for a fair monthly price.
Study more efficiently using our study tools.
Information
Topic
MedicineSubtopic
Medical Technology & SuppliesPeritoneal Dialysis
Suzuki H (ed): Home Dialysis in Japan.
Contrib Nephrol. Basel, Karger, 2012, vol 177, pp 3-12
Contrib Nephrol. Basel, Karger, 2012, vol 177, pp 3-12
______________________
A Kinetic Model for Peritoneal Dialysis and Its Application for Complementary Dialysis Therapy
Akihiro C. Yamashita
Department of Human Environmental Sciences, School of Engineering, Shonan Institute of Technology, Tsujido-Nishikaigan, Fujisawa, Kanagawa, Japan
______________________
Abstract
Kinetic models have been used in both hemodialysis (HD) and peritoneal dialysis (PD) therapies. Since many different theoretical models are available, users should choose one of these models along with the purpose of their studies. In general, simple models are useful for clinical investigations as well as clinical research, while rigorous models may be useful for engineers and cannot be utilized without an aid of computers. Several pieces of commercial software that include rigorous models are available for evaluation of peritoneal permeabilities as well as for constructing prescriptions. One of these pieces was clinically evaluated and high correlations with correlation coefficients >0.98 were found between clinical and recalculated values of total Kt/V for urea, total creatinine clearances and the ultrafiltration volume. Although the overall mass transfer-area coefficients (MTAC) of the peritoneal membrane is a diffusive parameter, it may become a useful tool for predicting peritoneal ultrafiltration by defining an index for peritoneal diffusive selectivity, the ratio of MTAC for urea to that for creatinine. It is recommended to use super high-flux dialyzers in PD+HD (complementary) combined therapy because it is the opportunity in a week to remove much middle and/or large molecules greater than ß2-microglobulin. Kinetic models are especially useful in treatments with relatively complex prescriptions such as PD+HD combined therapy, and may be a key to the further success of these modalities performed at home.
Copyright © 2012 S. Karger AG, Basel
There are several modalities available for treating end-stage renal disease patients. Each patient is required to choose one of these modalities after understanding features of each treatment. Peritoneal dialysis (PD) is used to be known as the first choice of the treatment because it was believed that PD could preserve the residual renal function (RRF) longer than hemodialysis (HD). However, since the choice of so-called super high-flux dialyzers that has high hydraulic permeability and high solute permeability as well as high biocompatibility [1] has become a standard with the use of ultrapure dialysis fluid [2], no significant difference has been reported in terms of preservation of RRF [3, 4]. Studies showed that local inflammation may greatly influence the preservation of RRF [5, 6]. There were so many factors that may directly or indirectly induce the local inflammation in classic HD treatment such as bioincompatibility of the dialysis membrane, water quality of dialysis fluid, etc.; however, most of these problems have already been solved in modern HD treatment. On the contrary, bioincompatibility of the dialysate for PD, including low pH, high glucose concentration and the existence of glucose degradation products, still remains a problem. Then there is the choice of PD as the initiation is becoming controversial for the purpose of preserving RRF.
Under such circumstances the choice of another modality is becoming more and more popular these days in Japan, that is, PD+HD combined therapy, also known as complementary dialysis recommended by an ad-hoc committee of the International Society for Peritoneal Dialysis (ISPD) in 2005. Although this modality is just a combination of PD and HD, the prescription may be even much more complicated than that for PD or for HD. This paper discusses a peritoneal transport model for PD and its application for complementary dialysis for the clinical use of prescription. How the kinetic model should be applied is also discussed for the further success of PD and PD-related modalities that are basically performed at home.
Theoretical
The first peritoneal transport model for PD was proposed by Henderson and Nolph [7], assuming only the diffusion would occur from the body compartment to the dialysate. Under such circumstances, the rate of mass transfer across the peritoneal membrane ṁ [mg/min] may be written in the following form:
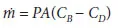 | (1) |
where Ρ is the peritoneal permeability [cm/min] and A is the effective surface area [cm2] of the peritoneal membrane, CB and CD are the concentrations in blood and dialysate (mg/ml), respectively. In this model, a uniform structure of the peritoneal membrane as well as no stagnant layer adjacent to it was taken into account. Considering these effects, Ρ should be replaced by the overall mass transfer coefficient Ko and equation 1 becomes:
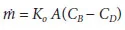 | (2) |
where the product of Ko and A is called the overall mass transfer-area coefficient (MTAC) [ml/min]. Babb et al. [8] and later Garred et al. [9] modified equation 2 by introducing convective mass transfer for small solutes from the blood to dialysate as follows:
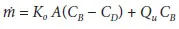 | (3) |
where Qu is the ultrafiltration rate across the peritoneum [ml/min]. Another modification was made by Yamashita and Hamada [10], co...
Table of contents
- Cover Page
- Front Material
- Introduction
- A Kinetic Model for Peritoneal Dialysis and Its Application for Complementary Dialysis Therapy
- How Automated Peritoneal Dialysis Is Applied and Maintained in Japan
- Introduction and Maintenance Program for PD Based on PD Guidelines for Japan
- Appropriate Drug Dosing in Patients Receiving Peritoneal Dialysis
- Surgical and Medical Treatments of Encapsulation Peritoneal Sclerosis
- Application of Peritoneal Dialysis in Elderly Patients by Classifying the Age into Young-Old, Old, and Oldest-Old
- Maintenance of Continuous Ambulatory Peritoneal Dialysis in Elderly Patients
- Role of Nurses in a Continuous Ambulatory Peritoneal Diagnosis Outpatient Clinic
- Combination Therapy with Hemodialysis and Peritoneal Dialysis
- Implementation of a Cooperative Program for Peritoneal Dialysis
- Care for Patients Carrying Out Dialysis Therapy at Home
- Perspectives on Home Hemodialysis in Japan
- Current International Status of Home Hemodialysis
- Future Home Hemodialysis - Advantages of the NxStage System One
- Introduction to Home Hemodialysis
- Overnight Home Hemodialysis: Eight Patients and Six Years of Experience in Sakairumi Clinics
- Practice of Home Hemodialysis in Dialysis Clinic
- Perspective of Home Hemodialysis in Japan
- Role of Clinical Engineers in Home Hemodialysis
- Daily Hemodialysis Improves Uremia-Associated Clinical Parameters in the Short Term
- Development of a Nanotechnology-Based Dialysis Device
- Author Index
- Subject Index
Frequently asked questions
Yes, you can cancel anytime from the Subscription tab in your account settings on the Perlego website. Your subscription will stay active until the end of your current billing period. Learn how to cancel your subscription
No, books cannot be downloaded as external files, such as PDFs, for use outside of Perlego. However, you can download books within the Perlego app for offline reading on mobile or tablet. Learn how to download books offline
Perlego offers two plans: Essential and Complete
- Essential is ideal for learners and professionals who enjoy exploring a wide range of subjects. Access the Essential Library with 800,000+ trusted titles and best-sellers across business, personal growth, and the humanities. Includes unlimited reading time and Standard Read Aloud voice.
- Complete: Perfect for advanced learners and researchers needing full, unrestricted access. Unlock 1.5M+ books across hundreds of subjects, including academic and specialized titles. The Complete Plan also includes advanced features like Premium Read Aloud and Research Assistant.
We are an online textbook subscription service, where you can get access to an entire online library for less than the price of a single book per month. With over 1.5 million books across 990+ topics, we’ve got you covered! Learn about our mission
Look out for the read-aloud symbol on your next book to see if you can listen to it. The read-aloud tool reads text aloud for you, highlighting the text as it is being read. You can pause it, speed it up and slow it down. Learn more about Read Aloud
Yes! You can use the Perlego app on both iOS and Android devices to read anytime, anywhere — even offline. Perfect for commutes or when you’re on the go.
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Yes, you can access Home Dialysis in Japan by H. Suzuki,H., Suzuki, Claudio Ronco,Claudio, Ronco in PDF and/or ePUB format, as well as other popular books in Medicine & Medical Technology & Supplies. We have over 1.5 million books available in our catalogue for you to explore.