Clinical Pathology of the Placenta
Martin Vogel, Gitta Turowski, Martin Vogel, Gitta Turowski
- 470 páginas
- English
- ePUB (apto para móviles)
- Disponible en iOS y Android
Clinical Pathology of the Placenta
Martin Vogel, Gitta Turowski, Martin Vogel, Gitta Turowski
Información del libro
This book performs a distinct introduction to the pathology of the placenta and its membranes, abortion material included, with the aim to facilitate and protect the quality of the morphological placental diagnostics by the pathologists. Seven chapters with coloured figures illustrating gross anatomy, development and maturation of the placenta explain the functional morphology in its clinical correlation of single and multiple findings for the pathologists, obstetricians and neonatologists. Moreover, the book contributes to a better understanding of pre- and perinatal investigations, maternal diseases, fetal outcomes and follow up of the newborns, as well as to the prevention of worse outcome in further pregnancies.
The atlas intends to stimulate the interest for perinatal pathology and to contribute to a better interdisciplinary understanding of pathologists and clinicians, midwives and nurses.
Preguntas frecuentes
Información
1 Normal anatomy and maturation
1.1 Anatomy and morphology
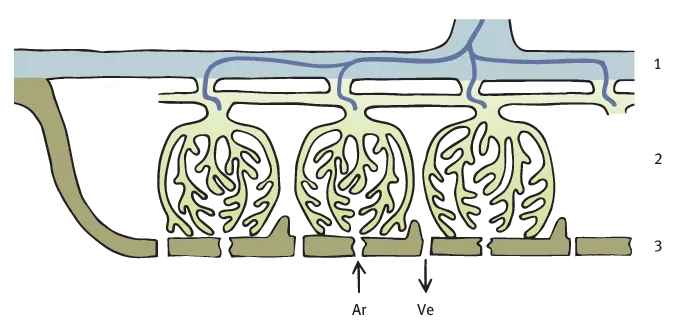
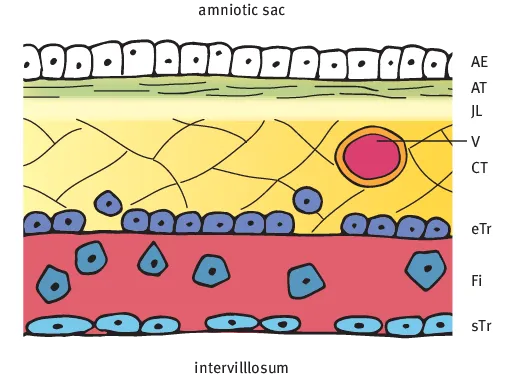
1.1.1 Chorionic plate
- – The Amniotic Epithelium (AE) layer covers the chorionic plate and forms the border of the amniotic sac.
- – The Amniotic collagenous Tissue (AT) layer differs in density depending on gestational age and contains collagenous fibers.
- – The Junctional Layer (JL) is a cell and fiber poor layer between the amniotic and chorionic connective tissue layers.
- – The Chorionic connective Tissue (CT) layer is fiber rich and cell poor. Embedded here are the chorionic plate vessel branches (V) which arise from the umbilical cord vessels and supply the stem villi.
- – The subchorionic layer of the Langhans-Fibrinoid (Fi) consists mainly of matrix-type fibrinoid and invasive cells of the extravillous trophoblast. The lamellar layer close to the intervillous space consists of fibrin-type fibrinoid.
- – Focal aggregates of extravillous Trophoblast cells (eTr) are seen at the base of the chorionic connective tissue layer and in the Langhans-fibrinoid layer. Syncytiotrophoblast cells (sTr) can be focally detected at the junction to the intervillous space.
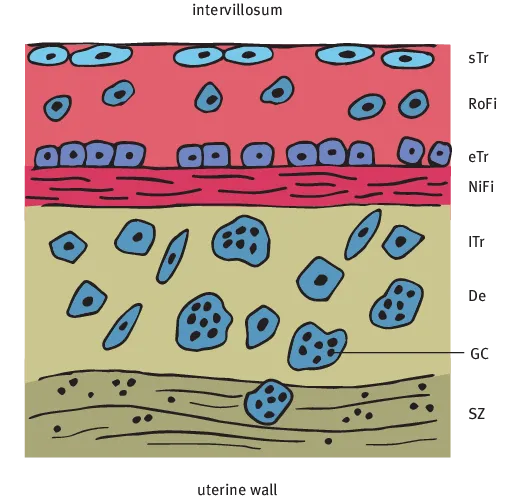
1.1.2 Basal plate
- 1. The extravillous trophoblast.
- 2. The maternal cells of the decidua basalis, soft tissue cells and leucocytes.
- 3. Fibrinoid.
- – Fibrin-type fibrinoid originating from coagulation processes and containing fibrin rich depositions and other maternal proteins.
- – Matrix-type fibrinoid secreted from extravillous trophoblast cells and containing fetal proteins.
- – The Rohr-Fibrinoid (RoFi) is seen next to the intervillous space and is infiltrated by non-proliferating trophoblast cells. A dense cell layer of basophilic Trophoblast cells (eTr) is seen underneath.
- – The Nitabuch-Fibrinoid (NiFi) layer is the point at which placental separation occurs at birth. This layer has a heterogeneous appearance and is comprised of connective tissue fibers, endometrial stromal cells and macrophages.
- – The Decidua basalis (De) contains stromal cells, macrophages, leucocytes and multinucleated Giant Cells (GC) of the extravillous and Intermediate trophoblast (Itr) types. Rudimentary fetal cells of the connecting stalk trophoblasts can also be found.
- – The Solution Zone (SZ) demarcates the uterus from the basal plate and contains the mucous decidual membrane that remains in the uterus following birth.
- – Vessel branches of the Spiral arteries (SP) transverse and branch within the basal plate and end in the intervillous space. One artery can have several fountain like openings in the central part of the fetal cotyledon [3]. Veins are extremely thin walled and often show sinusoidal dilatation.