![]()
CHAPTER 1
Defining Ethnic Dermatology: Challenges, Limitations, and Merits
Ophelia E. Dadzie
Department of Dermatology, North West London Hospitals NHS Trust and Centre for Clinical Science and Technology, University College London Division of Medicine, London, UK
Ethnic dermatology is a term used to describe an aspect of dermatology pertaining to individuals of diverse racial and ethnic backgrounds, who have richly pigmented skin and who share broadly similar cutaneous characteristics, notably the risk of scarring and dyspigmentation in response to cutaneous trauma. The term is analogous to skin of color, which is commonly used in North America. Defining the ethnic dermatology/skin of color cohort is challenging. However, broadly speaking and in this textbook, this cohort equates to individuals with Fitzpatrick skin phototypes (FSP) ІV–VІ and/or those of African, Asian, Middle Eastern, and/or Hispanic ancestry [1–2].
Unfortunately the use of terminologies such as ethnic dermatology and/or skin of color is not without its critics [3–4]. This is because of the problems and limitations of defining individuals by race, ethnicity, and/or skin pigmentation (an inherent problem in any scientific endeavor, which Richard Dawkins refers to as “the tyranny of the discontinuous mind”) [5]. Essentially humans do not fit into neat racial or ethnic categories, but represent a continuum. Thus, at what point does someone become “black” or “white”? Since evidence indicates that modern humans originate from Africa [6], are we not all of African ancestry? Furthermore, in advocating separating and defining specific groups based on racial, ethnic and/or skin pigmentation, are we contributing to a divisive society? After all, at a genetic level, humans share more similarities than differences [6]. In addition, the use of FSP has specific limitations when applied to pigmented skin (see Box 1.1 for discussion on this issue).
There is also a risk that terms such as ethnic dermatology will justify studies that use skin color and/or ethnicity to validate a biological construction of race that is actually rooted in socio-historical processes [7], e.g., “scientific studies” that supported the notion that people of African race are less prone to contact sensitization and hence better able to handle certain noxious substances [8].
All the above represent challenging questions and difficulties that we have had to navigate before embarking on this ethnic dermatology/skin of color “journey.” In response to these challenges we first have to consider the problems faced by practicing dermatologists.
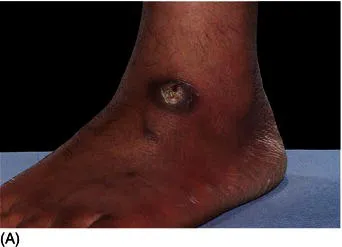
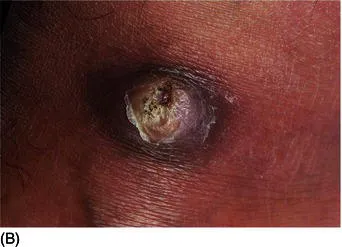
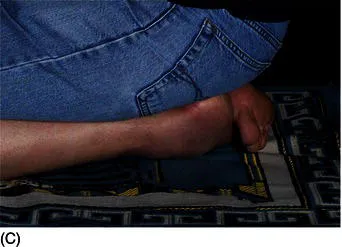
First, epidemiological studies and data obtained from hospital and/or private practices indicate that there are differences in the observed dermatoses in different ethnic/racial groups [9–10]. For instance, hair and scalp disorders are one of the major concerns in individuals with Afro-textured hair. Cultural factors also impact the range of dermatoses observed (e.g., the misuse of skin lightening agents in certain racial and/or ethnic groups and the occurrence of prayer nodules in Muslims [Fig. 1.1]). Thus, as practicing dermatologists, we need to be aware of these observed differences and the implications for managing our patients. Second, studies have highlighted deficiencies in dermatological educational resources and the training of dermatologists with regard to the field of skin of color/ethnic dermatology [11–12]. Finally, the demographics of most western countries is changing. This means that most practicing dermatologists need to be competent in the diagnosis and management of cutaneous disorders in people of diverse racial and ethnic backgrounds. For example, in 1990 the United States census revealed that 76% of the population was white; 12% black; 9% Hispanic; 2.8% Asian/Pacific Islander; and 0.7% American Indian, Eskimo, and Aleut [6]. Projections for the US population in 2050 forecast a substantial decline in the white population to approximately 53%, with an increase in other racial groups (black 14%; Hispanic 25%; Asian 8%; American Indian, Eskimo, and Aleut approaching 1%) [6]. In the United Kingdom, the 2001 census demonstrated that ethnic minorities made up 7.9% of the population, an increase of 53% compared to the previous 1991 census [13].
Box 1.1 Fitzpatrick skin phototype
The Fitzpatrick skin phototype (FSP) classification system (see also Box 1.2) [15] is used routinely by dermatologists to categorize and classify different skin types. It was initially developed by Thomas Fitzpatrick in 1975 to classify persons with “white skin” in order to select the correct initial dose of UVA for an upcoming large-scale oral PUVA photo-chemotherapy trial in the US in the mid-1970s. It was based primarily on a brief personal interview to evaluate individuals’ history of sunburn and tanning and not on phenotype (hair and eye color) [15]. The initial classification system placed all non-white/pigmented skin in one category, skin type V. Over time this classification system evolved and skin type V was divided into three sub-groups (IV, V, and VI) to encompass the diversity observed in those with pigmented skin. Furthermore, over time phenotype has had a greater impact on this classification system. It is the author’s opinion that often phenotype is the prime method used to categorize skin types, instead of proper evaluation of ultraviolet radiation response. This is one of the main limitations of FSP as a method of classifying individuals with pigmented skin. Furthermore, studies have shown a lack of a direct correlation between constitutive skin color and response to ultraviolet radiation. For instance, individuals originating from various Asian countries encompass a diverse group and skin color does not always predict their skin phototypes [16,17]. Another limitation of FSP is that it is based on self-reported erythema sensitivity and tanning ability, and hence it is not quantitative or reliable. Furthermore, it cannot be applied for in vitro conditions. For this reason, new classification systems have been developed, such as the colorimetric classification of constitutive pigmentation by individual typology angle [18,19] and the Roberts skin classification system [20] (Box 1.2). The former is of relevance in the research setting, while the latter is of practical relevance in predicting response to trauma, prior to procedural dermatology. There are four elements to the Roberts skin classification system, which should be evaluated based on a thorough history, examination, and evaluation of test site reaction.
Box 1.2 Roberts skin type classification system
Fitzpatrick (FZ) scale: measures skin phototype
FZ1 White skin. Always burns, never tans
FZ2 White skin. Always burns, minimal tan
FZ3 White skin. Burns minimally, tans moderately and gradually
FZ4 Light brown skin. Burns minimally, tans well
FZ5 Brown skin. Rarely burns, tans deeply
FZ6 Dark brown/black skin. Never burns, tans deeply
Roberts hyperpigmentation (H) scale: propensity for pigmentation
H0 Hypopigmentation
H1 Minimal and transient (< 1 year) hyperpigmentation
H2 Minimal and permanent (> 1 year) hyperpigmentation
H3 Moderate and transient (< 1 year) hyperpigmentation
H4 Moderate and permanent (> 1 year) hyperpigmentation
H5 Severe and transient (< 1 year) hyperpigmentation
H6 Severe and permanent (> 1 year) hyperpigmentation
Glogau (G) scale: describes photoaging
G1 No wrinkles, early photoaging
G2 Wrinkles in motion, early to moderate photoaging
G3 Wrinkles at rest, advanced photoaging
G4 Only wrinkles, severe photoaging
Roberts scarring (S) scale: describes scar morphology
S0 Atrophy
S1 None
S2 Macule
S3 Plaque within scar boundaries
S4 Keloid
S5 Keloidal nodule
Based on the above and despite the valid limitations and difficulties in defining ethnic dermatology, the use of this term is helpful, given that it enables interested parties (dermatologists, other physicians, nurses, scientists, and patients) to come together to help advance this aspect of dermatology [2]. In time it is likely that advances in genomics will increase our understanding of the role of genetic variation among human populations, thereby influencing our use of terminologies such as ethnic dermatology and skin of color [14].
References
1 Dadzie OE. Skin of colour: an emerging subspecialty of Dermatology. Br J Dermatol 2009; 160: 368–75.
2 Taylor SC, Cook-Bolden F. Defining skin of color. Cutis 2002; 69: 435–7.
3 Silver SE. Defining skin of color. Cutis 2003; 71: 141–2; author reply 142–3; discussion 143.
4 Elgart ML. Defining sk...