Foot problems in diabetic patients are some of the most challenging complications to treat, due to an often quite late presentation of symptoms from the patient. Therefore visual recognition of presenting clinical signs is absolutely key for a successful diagnosis and subsequently, the right management programme.
The 3rd edition of Managing the Diabetic Foot once again provides a practical, handy and accessible pocket guide to the clinical management of patients with severe feet problems associated with diabetes, such as ulcers, infections and necrosis. By focusing on the need for a speedy response to the clinical signs, it will enable doctors make rapid, effective management decisions in order to help prevent deterioration and avoid the need for evental foot amputation.
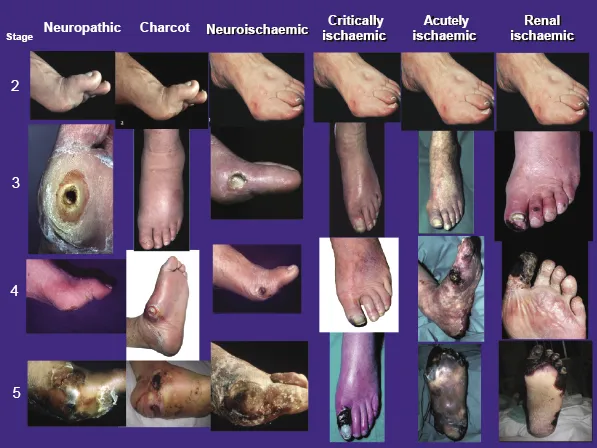
Each chapter focuses specifically on the different stages of foot disease and the clinical management required at that particular stage, ie, the normal foot; high-risk foot, ulcerated foot, infected foot, necrotic foot and unsalvageable foot.
Full colour throughout, it will feature over 150 clinical photos, numerous hints and tips to aid rapid-reference, as well as the latest national and international guidelines on diabetic foot management.
Managing the Diabetic Foot, 3E, is the ideal go-to clinical tool for all diabetes professionals, specialist diabetes nurses and podiatrists managing patients with diabetic foot problems.