
- 162 pages
- English
- ePUB (mobile friendly)
- Available on iOS & Android
eBook - ePub
Human Microbial Ecology
About this book
The aim of this comprehensively written volume is to provide a baseline of information on the normal microflora at various sites in the body. It focuses on the mouth, upper digestive tract, large intestine, skin, and urinogenital tract. Written in an easy-to-read format, this book highlights the level of detail available. For example, it explains that in the mouth and colon the data are extremely detailed and good quantitative information is available on large numbers of bacterial species. This work analyzes the similarities and differences between the microfloras of the various "internal" surfaces, and discusses the clear value of good taxonomy. It focuses on problems and extended research in the progress at other sites. Because this work researches the advances and discoveries made in specific areas of human microbial ecology, it is an ideal source for all who are involved in microbiology, bacteriology, and infectious diseases.
Trusted by 375,005 students
Access to over 1 million titles for a fair monthly price.
Study more efficiently using our study tools.
Information
Subtopic
BiologyIndex
Biological SciencesChapter 1
FACTORS CONTROLLING THE MICROFLORA OF THE HEALTHY MOUTH
Else Theilade
TABLE OF CONTENTS
I. Introduction
II. Oral Habitats
III. The Normal (Resident) Oral Microflora of Man
A. Definition
B. The Resident Oral Microflora
C. Transient Oral Microflora
D. The Oral Microflora in Health and Disease
IV. Methods of Studying the Oral Microflora
A. Sampling
B. Transport and Suspension of Samples
C. Examination By Microscopy
D. Cultural Studies
V. Microorganisms of the Resident Oral Microflora
VI. The Microflora of the Major Oral Habitats
A. Mucosal Surfaces
B. Teeth and Artificial Structures
VII. Adherence and Retention of Microorganisms in the Mouth
VIII. Growth Conditions and Sources of Nutrients
A. Oral pH
B. Anaerobiosis
C. Nutrients
IX. Microbial Interactions among the Oral Microflora
X. Regulation by Host Defense Mechanisms
XI. Acquisition and Development
XII. Effect of Antimicrobial Agents
XIII. Conclusion
References
I. INTRODUCTION
Microorganisms from the mouth were first observed in 1683 by Antonie van Leeuwenhoek using his newly developed microscope. No significance was, however, ascribed to them at that time. When Pasteur had established the foundation of modern microbiology, Miller,1 in 1890, reported on his pioneer studies and put forward hypotheses which still hold on the role of oral bacteria in the aetiology of dental caries and periodontal diseases.1 The inspiration of Scherp (1908—1974) in education and research guided us on to fruitful investigations of the ecology of the oral microbiota and the complex host-microbial interactions prevailing in the mouth. The oral microflora is beneficial for the host, mainly by acting as a barrier against exogenous microorganisms. Thus, long-term antibiotic therapy may suppress the normal oral flora and give rise to overgrowth by, for example, enteric bacteria. Another useful function may be the production of vitamins B and K. On the other hand imbalances in the normal oral microflora may lead to oral diseases such as dental caries and periodontal diseases which are very prevalent and costly to treat. Oral microorganisms also cause opportunistic infections of oral soft tissues and bones (“dental abscesses”) and sometimes even spread to remote parts of the body giving rise to infective endocarditis or abscesses of lung, liver, or brain. During the past 30 years, numerous investigators around the world have contributed to an explosive increase in information about the oral ecosystems in health and disease. The oral microflora and its interactions are, however, far more complex than anticipated, and much research remains to be done.
II. ORAL HABITATS
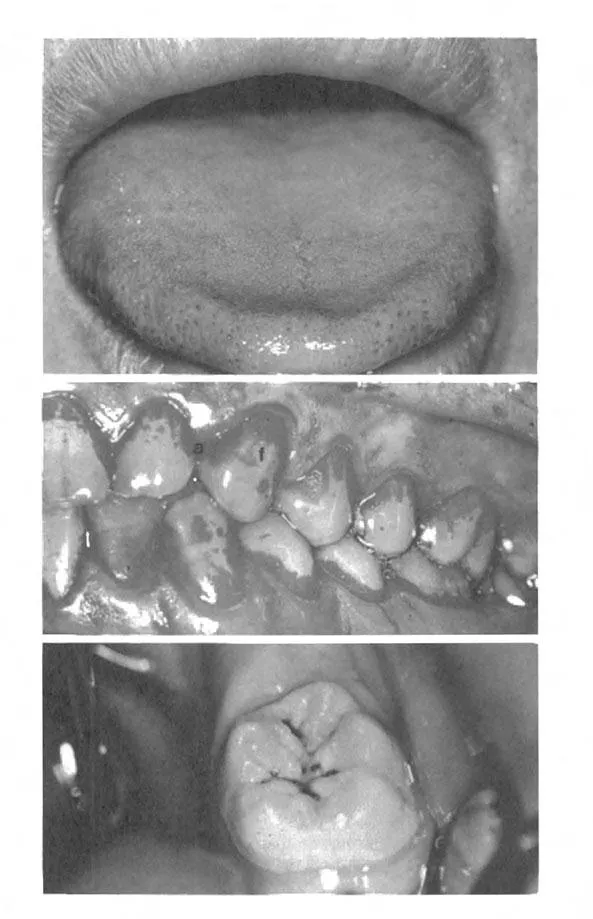
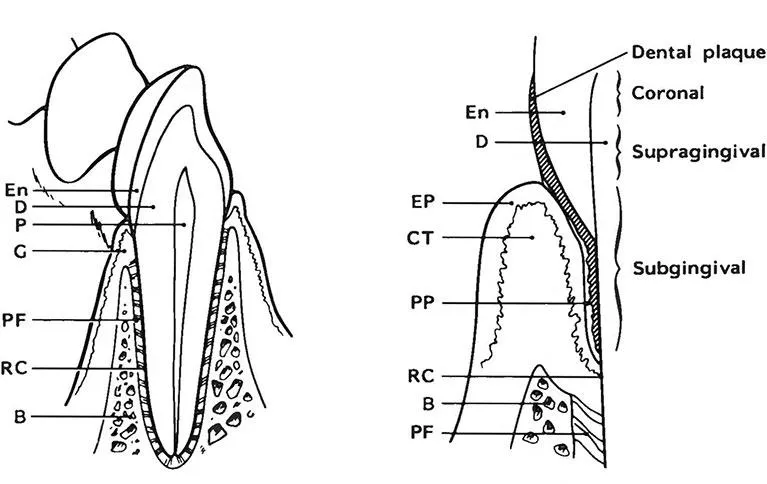
The oral ecosystem consists of the oral microorganisms and the surroundings in which they live, i.e., the mouth. There are several different oral habitats where microorganisms can grow. Each habitat is populated by a characteristic community consisting of populations of various species, with each species filling a niche (a certain functional role) in the community.2,3 In order to remain in the mouth the microorganisms must adhere to the oral surfaces and resist being eliminated with the stream of saliva being swallowed, and grow under the different conditions prevailing at the various sites (Figures 1 and 2). The mucosal surfaces are characterized by a rapid cell turnover with continuous desquamation of the superficial epithelial cells and the microflora colonizing them. Only the papillary upper surface of the tongue has sufficient retention sites to harbor numerous microorganisms; generally, the numbers are smaller on the smooth oral mucosa of palate, gingiva, lips, cheeks, and floor of the mouth. The tonsils are usually not considered to be part of the mouth, but may act as reservoir for some dental plaque bacteria. The hard, nonshedding surfaces of teeth, fillings, artificial crowns, and dentures have a large potential for massive and long-lasting colonization (termed dental plaque), unless they are kept clean by oral hygiene. Special retentive areas, not exposed to mechanical friction during function, are occlusal fissures, approximal tooth surfaces, gingival pockets, and the fitting surface of artificial dentures4 (see later). Such sites can harbor extremely numerous and complex microbial communities, and are described below. Saliva flowing over the oral surfaces becomes contaminated with microorganisms from the various habitats, mainly from the large surface of the dorsum of the tongue.
III. THE NORMAL (RESIDENT) ORAL MICROFLORA OF MAN
A. DEFINITION
All the microorganisms which establish a more or less permanent residence at oral surfaces in man, in one or more of the oral habitats, are referred to as normal microflora (or normal microbiota) of the human mouth.5 Expressions such as resident, indigenous, autochthonous, or commensal microflora are used with a similar meaning. Probably “resident oral microflora” expresses the intended meaning most simply and without implying the possible useful or harmful effects which the microflora may have on the host. From an ecological point of view it is natural to include all microorganisms which have the mouth as their primary habitat in the resident oral flora, although they are not necessarily present in all mouths all the time. In fact, some resident oral microorganisms are dependent on special oral habitats, which are not always present, such as teeth or artificial hard surfaces (for Streptococcus mutans), and gingival crevices or pockets (for spirochaetes and some Gramnegative rods).6 Microorganisms qualify as members if they occupy a particular niche in the oral microflora and are frequently isolated fro...
Table of contents
- Cover
- Title Page
- Copyright Page
- Introduction
- The Editors
- Advisory Board
- Contributors
- Table of Contents
- Chapter 1 Factors Controlling the Microflora of the Healthy Mouth
- Chapter 2 Factors Controlling the Microflora of the Healthy Upper Gastrointestinal Tract
- Chapter 3 Control of the Large Bowel Microflora
- Chapter 4 Factors Affecting the Microflora of the Lower Genital Tract of Healthy Women
- Chapter 5 Factors Controlling the Microflora of the Skin
- Index
Frequently asked questions
Yes, you can cancel anytime from the Subscription tab in your account settings on the Perlego website. Your subscription will stay active until the end of your current billing period. Learn how to cancel your subscription
No, books cannot be downloaded as external files, such as PDFs, for use outside of Perlego. However, you can download books within the Perlego app for offline reading on mobile or tablet. Learn how to download books offline
Perlego offers two plans: Essential and Complete
- Essential is ideal for learners and professionals who enjoy exploring a wide range of subjects. Access the Essential Library with 800,000+ trusted titles and best-sellers across business, personal growth, and the humanities. Includes unlimited reading time and Standard Read Aloud voice.
- Complete: Perfect for advanced learners and researchers needing full, unrestricted access. Unlock 1.4M+ books across hundreds of subjects, including academic and specialized titles. The Complete Plan also includes advanced features like Premium Read Aloud and Research Assistant.
We are an online textbook subscription service, where you can get access to an entire online library for less than the price of a single book per month. With over 1 million books across 990+ topics, we’ve got you covered! Learn about our mission
Look out for the read-aloud symbol on your next book to see if you can listen to it. The read-aloud tool reads text aloud for you, highlighting the text as it is being read. You can pause it, speed it up and slow it down. Learn more about Read Aloud
Yes! You can use the Perlego app on both iOS and Android devices to read anytime, anywhere — even offline. Perfect for commutes or when you’re on the go.
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Yes, you can access Human Microbial Ecology by Michael J. Hill,Philip D. Marsh in PDF and/or ePUB format, as well as other popular books in Biological Sciences & Biology. We have over one million books available in our catalogue for you to explore.