![]()
1
Introduction to Treatment of Autism Spectrum Disorder (ASD)
Patricia A. Prelock and Rebecca J. McCauley
INTRODUCTION
This book is intended to introduce readers who have some familiarity with autism spectrum disorder (ASD) and its core impairments to a group of interventions focused on social communication and social interaction. Because the diagnostic category for autism has undergone modification since the first edition of this text, this chapter describes these changes and briefly highlights some implications for these changes. The chapter then provides updates on national reviews of interventions considered to be established in support of the social communication and social interaction of children with ASD.
CHANGES TO THE DSM-5
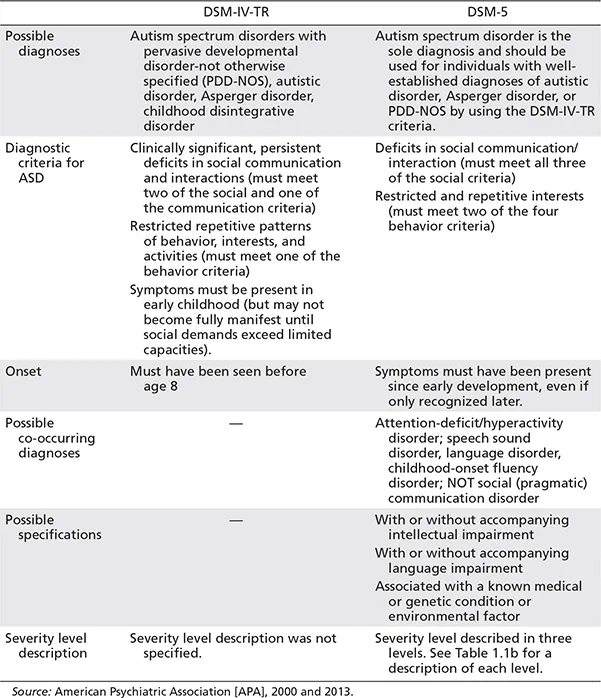
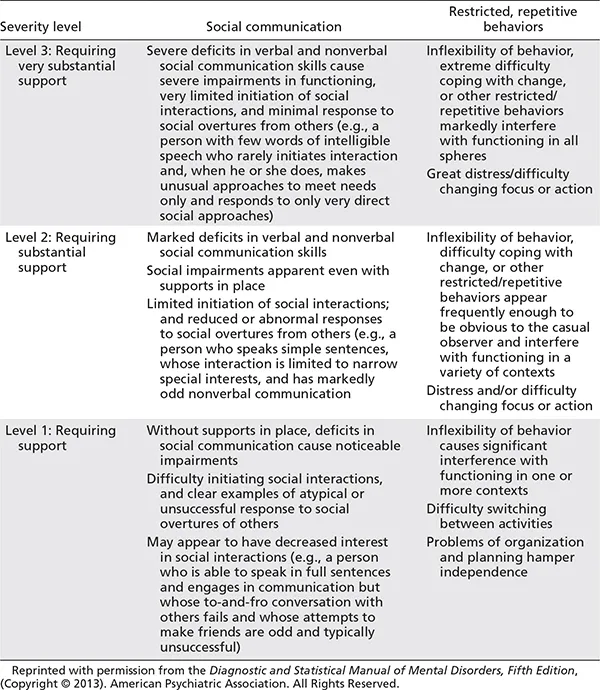
When the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition-Text Revision (DSM-IV-TR; American Psychiatric Association [APA], 2000) was updated to DSM-5 (APA, 2013), pervasive developmental disorder/autism, with its subthreshold diagnoses, changed to autism spectrum disorder. The diagnostic criteria also moved from three primary diagnostic categories to two: 1) social communication and social interaction and 2) restricted, repetitive, and stereotyped patterns of behavior. Expansion within each category also occurred. Table 1.1a summarizes differences between the earlier (DSM-IV-TR, APA, 2000) and the current characterization of ASD (DSM-5; APA, 2013). A particularly significant change is that language and cognition are now considered to be potential comorbid conditions and require a separate assessment to ensure deficits in these areas cannot be better explained by an intellectual disability (ID) or a global developmental delay. Table 1.1b describes the severity levels now associated with each of the two primary diagnostic categories (DSM-5; APA, 2013).
![]()
Table 1.1a. A summary of changes associated with autism spectrum disorder (ASD) diagnoses based on the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition-Text Revision (DSM-IV-TR; American Psychiatric Association [APA], 2000) and Fifth Edition (DSM-5; APA, 2013)
![]()
Table 1.1b. Severity levels associated with the two diagnostic criteria for autism spectrum disorder in the DSM-5
![]()
Several implications are discussed in the literature regarding the application of the new DSM-5 criteria. For example, Young and Rodi (2014) found only 57.1% of those with pervasive developmental disorders (PDDs) on the DSM-IV met the criteria for DSM-5, whereas 50%–75% maintained diagnoses in a review completed by Smith and colleagues (2015). In both studies, children with a diagnosis of PDD-not otherwise specified (PDD-NOS) and Asperger’s disorder were less likely to meet the DSM-5 criteria, specifically all three social communication and social interaction criteria. However, a case was made to ensure students who may not qualify under the new criteria continue to receive the intervention services they require (Smith et al., 2015; Young & Rodi, 2014).
A study with 185 children under 5 years old indicated that children with autism on the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR; APA, 2000) were also diagnosed with ASD on the DSM-5, but children with previous PDD-NOS diagnoses had fewer comorbid and emotional behaviors and insufficient symptoms in the restricted repetitive patterns of behavior category to qualify for an ASD diagnosis (Christiansz et al., 2016). Another study (Zander & Bolte, 2015) of younger children between 20 and 47 months found that 12%–67% of the children who met the DSM-IV-TR criteria did not meet the DSM-5 criteria, although diagnosis was influenced by severity level, leading to less consistent diagnosis. Reports by the Centers for Disease Control and Prevention (Baio et al., 2018), however, indicate the number of children meeting the DSM-5 criteria for ASD as compared to the DSM-IV-TR criteria are fairly similar, with DSM-IV-TR cases exceeding DSM-5 cases by less than 5% and with an 86% overlap between the two definitions. It remains unclear what the impact has been or will be to the prevalence of ASD diagnoses with the addition of social communication disorder (APA, 2013). Although this disorder is characterized by challenges in the social use of both verbal and nonverbal communication similar to ASD, there is no evidence of restricted and repetitive patterns of behaviors, interests, or activities. Whatever the ultimate impact is of the application of the DSM-5 on the diagnosis of ASD, children still require evidence-based interventions that address their social communication and social interaction impairments, as prevalence numbers continue to rise with 1 in 59 children receiving a diagnosis (Baio et al., 2018).
BACKGROUND ON INTERVENTION STRATEGIES FOR COMMUNICATION AND SOCIAL INTERACTION
Since 2000, thinking has evolved about which intervention approaches are most appropriate for supporting the social interaction and communication needs of children with ASD as well as children with social pragmatic disorders who may not meet the ASD diagnosis. Although traditional behavioral interventions are plentiful in the literature (e.g., Cooper et al., 2007) and tremendously influential in a variety of settings (Downs et al., 2007; Lafasakis & Sturmey, 2007; Taubman et al., 2001), social-pragmatic developmental interventions continue to gain traction, including those that involve parent training, in part because they emphasize opportunities for people with ASD to establish positive social connections and generalize their skills in the natural environment. Interest in these approaches has also arisen in response to limitations identified in traditional behavioral approaches to ASD in terms of generalization of targeted behaviors, particularly those related to the social use of communication and language (Wetherby & Woods, 2006, 2008). This book focuses primarily on such approaches because of their special promise in addressing the social communication and social interaction challenges at the core of ASD and their potential to minimize barriers to the functional application of learning.
In the traditional behavioral approach, practitioners teach skills one-to-one with a predetermined correct response (Karsten & Carr, 2009; Newman et al., 2009; Prelock & Nelson, 2012) and a highly prescribed teaching structure (e.g., discrete trial training [Cooper et al., 2007]). In contrast, in a social-pragmatic developmental approach, the interventionist follows the child’s lead, fosters initiation and spontaneity, and reinforces contingent responses. Several strategies consistent with these approaches have long been implemented as part of naturalistic communication and language interventions for children with a variety of communication and language challenges (Girolametto et al., 1996; Kaiser et al., 2000; Kaiser & Hester, 1994) and have more recently been elaborated upon and modified to address the special challenges presented by ASD.
Several of the interventions described in this text capitalize on the value of integrating the best of behavioral and developmental approaches to achieve functional and relevant social and communicative outcomes for children, adolescents, and adults with ASD. For example, Prizant and Wetherby (1998), recognizing the contributions of both a traditional behavioral and older developmental approaches to intervention, proposed contemporary behavioral interventions (i.e., middle ground interventions) to support the communication and social interaction needs of children with ASD. In particular, they described the value of giving children choices, sharing communication opportunities between the interventionist and the child, and using preferred activities and materials—strategies that characterize pivotal response training (Koegel, Koegel, Harrower, & Carter, 1999; Koegel, Koegel, Shoshan, & McNerney, 1999).
As intervention approaches have evolved, so too have comprehensive guidelines for best practices. In 2001, the National Research Council (NRC) offered a description of best practices for children with ASD through the early childhood years. A number of intervention guidelines emerged from a comprehensive review of the literature, including initiating treatment as soon as possible; ensuring active engagement during intensive instruction; using developmentally appropriate, goal-based, and systematically planned activities; implementing planned teaching opportunities throughout the day; and involving families and peers in the intervention to facilitate generalized skill learning. Many early intervention programs have used these best practices to design comprehensive educational programs for young children with ASD.
As a follow-up to the NRC (2001) description, Iovannone and colleagues (2003) proposed six educational practices as appropriate and effective for school-age children with ASD: 1) providing individualized supports and services that matched a student’s profile as defined through the individualized education program (IEP) process; 2) offering systematic, carefully planned, and defined instructional procedures to achieve valid goals with a process for measuring outcomes; 3) creating a structured learning environment; 4) adding specialized curriculum content in the area of social engagement and recreation and leisure skills; 5) defining a functional approach to problem behaviors; and 6) engaging families in their student’s educational success. Challenges remained, however, in determining the most effective instructional procedures for children of varying ages, language abilities, and cognitive levels with diagnoses of autism and subthreshold diagnoses, such as Asperger syndrome and PDD-NOS.
To address the gaps in the intervention effectiveness literature for the large heterogeneous group of children with ASD, in 2009 the National Autism Center (NAC) (https://www.nationalautismcenter.org) released a report of a comprehensive review of 775 intervention studies since 1957. In that report, the authors categorized the current level of evidence for several interventions typically used in the treatment of individuals with ASD...