Providing a solid foundation in the normal development of functional movement, Functional Movement Development Across the Life Span, 3rd Edition helps you recognize and understand movement disorders and effectively manage patients with abnormal motor function. It begins with coverage of basic theory, motor development and motor control, and evaluation of function, then discusses the body systems contributing to functional movement, and defines functional movement outcomes in terms of age, vital functions, posture and balance, locomotion, prehension, and health and illness. This edition includes more clinical examples and applications, and updates data relating to typical performance on standardized tests of balance. Written by physical therapy experts Donna J. Cech and Suzanne "Tink" Martin, this book provides evidence-based information and tools you need to understand functional movement and manage patients' functional skills throughout the life span.- Over 200 illustrations, tables, and special features clarify developmental concepts, address clinical implications, and summarize key points relating to clinical practice.- A focus on evidence-based information covers development changes across the life span and how they impact function.- A logical, easy-to-read format includes 15 chapters organized into three units covering basics, body systems, and age-related functional outcomes respectively.- Expanded integration of ICF (International Classification of Function) aligns learning and critical thinking with current health care models.- Additional clinical examples help you apply developmental information to clinical practice.- Expanded content on assessment of function now includes discussion of participation level standardized assessments and assessments of quality-of-life scales.- More concise information on the normal anatomy and physiology of each body system allows a sharper focus on development changes across the lifespan and how they impact function.

eBook - ePub
Functional Movement Development Across the Life Span
- 374 pages
- English
- ePUB (mobile friendly)
- Available on iOS & Android
eBook - ePub
Functional Movement Development Across the Life Span
About this book
Trusted by 375,005 students
Access to over 1 million titles for a fair monthly price.
Study more efficiently using our study tools.
Information
Unit Two
Body Systems Contributing to Functional Movement
Chapter 6 Skeletal System Changes
Objectives
After studying this chapter, the reader will be able to:
1. Describe the structures and components of the skeletal system.
2. Identify the function of bone and cartilage in supporting posture and movement.
3. Discuss unique structural and functional characteristics of the skeletal system in the developing fetus, infant, child, adolescent, adult, and older adult.
4. Relate the age-related characteristics of the skeletal system to functional movement abilities and risk factors.
5. Incorporate consideration of life span development of the skeletal system into patient assessment and treatment planning.
The ability to walk, run, lift, and manipulate objects is influenced by the strength and resilience of the skeletal system. A young infant cannot walk, climb stairs, push a stroller, or tie shoes. Not only do infants lack the experience and practice necessary for these tasks, their immature skeleton does not provide a structural framework on which these movements can take place. Older adults may not have the spring in their step, power in their tennis serve, or manual dexterity they enjoyed when they were younger. The changes in the skeletal system that occur with aging may contribute to decreased efficiency of movement. Across the life span, the skeletal system evolves and influences our ability for unrestricted movement.
The skeletal system, as discussed in this chapter, consists of the bony skeleton and cartilage. The skeleton provides a structure on which muscles can work. The size and shape of the bones, mechanics of joint articulations, and location of muscular attachments form an efficient system of levers and struts. Joints allow bones to articulate with each other, and the shape of the joint contributes to efficiency of movement. Cartilage acts as a shock absorber and protects joint surfaces from wear and tear. We better appreciate the contribution of the skeletal system to functional movement when we understand the role of its components and their changing properties throughout development.
Components of the skeletal system
Cartilage
Cartilage, a type of connective tissue, can tolerate mechanical stress and acts as a supporting structure in the body. It provides a mechanism for shock absorption, acts as a sliding surface for the joints, and plays a role in the development and growth of bone. During fetal development, a cartilage model is laid down from which the long bones of the body will develop. The ends of immature long bones and some sites of muscular attachment also contain cartilage plates, which are sites of bone growth.
Three types of cartilage exist, each meeting different functional needs (Figure 6-1). Hyaline cartilage is the most abundant and rigid. It is found at the articular surfaces of joints and the walls of respiratory passages, such as the trachea and bronchi. Hyaline cartilage also makes up the fetal model of the future long bones and can be found at the epiphyseal growth plates of immature bone. Fibrocartilage is found at the acetabulum, intervertebral disks, menisci, and tendinous insertions. It is more pliable than hyaline cartilage but still provides strength and support to the skeletal system. Fibrocartilage fibers are arranged parallel to the stress forces that the tissue experiences. Elastic cartilage is the most pliable cartilage and can be found at the larynx, ear, and epiglottis, where it provides support with flexibility.
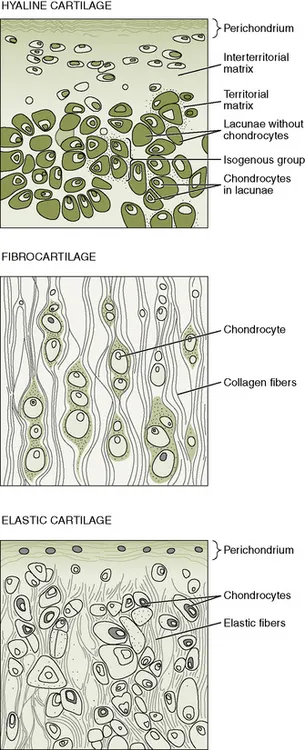
Figure 6-1 Diagram of the types of cartilage.
(From Gartner LP, Hiatt JL: Color textbook of histology, ed 2, Philadelphia, 2001, WB Saunders, p 130.)
Hyaline cartilage covers the ends of the bones that make up synovial joints, and in this capacity, it is called articular cartilage. It is responsible for facilitating motion at the joints and can tolerate a variety of loading forces. Synovial fluid and the compression of fluids from within the surface of the articular cartilage contribute to lubrication of the joint. Articular cartilage provides a low friction surface and allows joints to move freely through older adulthood.1,2 Years of microtrauma, isolated instances of more severe joint trauma, and aging of the cartilaginous tissue eventually result in a breakdown of articular cartilage, which contributes to the development of osteoarthritis for many older adults.
Properties
Cartilage consists of water, proteoglycans, collagen fibers, and cartilage cells (chondrocytes). The proteoglycans and collagen fibers make up the extracellular collagen matrix surrounding the chondrocytes. Differences in the extracellular matrix and amount of water in the tissue help to differentiate the three types of cartilage. For example, the water content of articular cartilage is 60% to 80%2 but that of fibrocartilage is only 50%.1 The collagen matrix contributes to the stiffness and resilience of the collagen and helps to bind water within the cartilage.3
Cartilage has no nerve supply and no vascular supply of its own. Oxygen and nutrients must be obtained from surrounding tissues. Most cartilage is covered by a layer of dense connective tissue called the perichondrium. The perichondrium is vascularized and supplies nutrients to the cartilage via diffusion. Articular cartilage is not covered with perichondrium and depends on diffusion of nutrients from synovial fluid and subchondral bone. In articular cartilage, periods of compression and decompression facilitate the exchange of fluids: during decompression, osmotic forces allow nutrients to diffuse into the cartilage, and during compression, fluids and waste products can be squeezed out.1,4 Both processes are necessary to maintain adequate nutrition of the cartilage. Health of the articular cartilage is promoted through use, or the loading of the cartilage.5
In the absence of mechanical loading, atrophy of the articular tissue may be seen. The atrophied articular cartilage may be less able to withstand weight-bearing and movement forces, leading to further degeneration of the cartilage.3,5
Formation
Cartilage is derived from embryonic mesoderm, as is other connective tissue. Cartilage growth occurs through two different processes: interstitial growth and appositional growth. Interstitial growth occurs within the cartilage through mitotic division of the existing chondrocytes. It occurs in the early phases of cartilage development to increase tissue mass, at the epiphyseal plates of long bones, and at articular surfaces. In appositional growth, new cartilage is laid down at the surface of the perichondrium. In this process, chondroblasts of the perichondrium, which are precursors to chondrocytes, form an extracellular matrix and develop into mature chondrocytes. Nonarticular cartilage loses the capacity for interstitial growth early and then undergoes only appositional growth.
In the formation of articular cartilage, collagen fibers of the extracellular matrix weave together and form a loop parallel to the joint surface. These collagen fibers are embedded in the subchondral bone or deep...
Table of contents
- Cover
- Title Page
- Front matter
- Copyright
- Dedication
- Contributors
- Preface
- Acknowledgments
- Table of Contents
- Unit One: Definition of Functional Movement
- Unit Two: Body Systems Contributing to Functional Movement
- Unit Three: Functional Movement Outcomes
- Index
Frequently asked questions
Yes, you can cancel anytime from the Subscription tab in your account settings on the Perlego website. Your subscription will stay active until the end of your current billing period. Learn how to cancel your subscription
No, books cannot be downloaded as external files, such as PDFs, for use outside of Perlego. However, you can download books within the Perlego app for offline reading on mobile or tablet. Learn how to download books offline
Perlego offers two plans: Essential and Complete
- Essential is ideal for learners and professionals who enjoy exploring a wide range of subjects. Access the Essential Library with 800,000+ trusted titles and best-sellers across business, personal growth, and the humanities. Includes unlimited reading time and Standard Read Aloud voice.
- Complete: Perfect for advanced learners and researchers needing full, unrestricted access. Unlock 1.4M+ books across hundreds of subjects, including academic and specialized titles. The Complete Plan also includes advanced features like Premium Read Aloud and Research Assistant.
We are an online textbook subscription service, where you can get access to an entire online library for less than the price of a single book per month. With over 1 million books across 990+ topics, we’ve got you covered! Learn about our mission
Look out for the read-aloud symbol on your next book to see if you can listen to it. The read-aloud tool reads text aloud for you, highlighting the text as it is being read. You can pause it, speed it up and slow it down. Learn more about Read Aloud
Yes! You can use the Perlego app on both iOS and Android devices to read anytime, anywhere — even offline. Perfect for commutes or when you’re on the go.
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Yes, you can access Functional Movement Development Across the Life Span by Donna Joy Cech,Suzanne Tink Martin,Donna J. Cech,Suzanne "Tink" Martin in PDF and/or ePUB format, as well as other popular books in Medicine & Physiotherapy, Physical Medicine & Rehabilitation. We have over one million books available in our catalogue for you to explore.