![]()
CORNEA
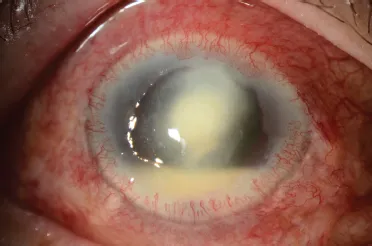
| 1. | A 24-year-old contact lens wearer comes in with a two-day history of eye pain. |
Figure 1.1
| Q | 1.1 What else do you want to know about in the history? |
•Blurring of vision
•Contact lens history
•Contact with soil or contaminated water
•Immunosuppression: diabetes, human immunodeficiency virus, steroids, chemotherapy onset
•Progression
•Previous treatment
•Pain
•Trauma
| Q | 1.2 What are the signs? |
•Conjunctiva: injected
•Corneal ulcer/infiltrate involving the visual axis
•Central epithelial defect
•Hypopyon
| Q | 1.3 What are your differential diagnoses? |
•Contact lens-related infective keratitis
•Exposure infective keratitis/neurotrophic infective keratitis
| Q | 1.4 How do you manage the above patient? |
•Admit the patient
•Perform a corneal scrape and send for microscopy and cultures
•Intensive topical antibiotic treatment: gentamicin 14 mg/ml hourly, cephazolin 50 mg/ml hourly through the night
•Systemic antibiotic treatment if the infiltrate is near the limbus (oral ciprofloxacin 500 mg twice a day for a week)
| Q | 1.5 What do you send the corneal scrapings for? |
•Gram stain
•Blood agar
•Chocolate agar
•Thioglycate
•Brain heart infusion broth (BHIB)
•Sabouraud dextrose
•Others
⚬Suspicious for fungal infection: giemsa stain, methenamine silver stain
| Q | 1.6 What are the complications of a corneal ulcer? |
•Acute: thinning of the cornea resulting in corneal perforation leading to endophthalmitis
•Long-term: scar, astigmatism, blindness