![]()
Assessment Paper
1
Question 1.1
A 40-year-old male presents with painful swelling of the right knee of three days’ duration. He denied prior history of joint pain. He had been on a recent business trip to Batam where he consumed more than his usual intake of alcohol and seafood.
1A. Give three most likely differential diagnoses.
(3 marks)
a. ...............................................................................................
b. ...............................................................................................
c. ...............................................................................................
1B. List three most important specific aspects of history that you would like to ask.
(3 marks)
a. ...............................................................................................
b. ...............................................................................................
c. ...............................................................................................
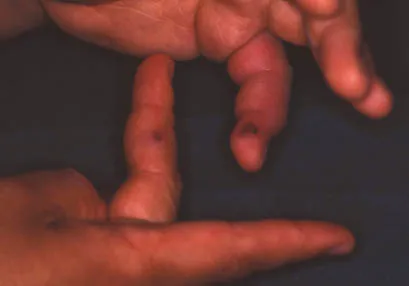
On examination, he is afebrile and has a warm right knee with effusion with almost zero range of motion. The left elbow and ankle are tender without any redness or swelling. Some skin lesions are seen on his hands.
2A. Describe the lesions seen.
(2 marks)
...................................................................................................
2B. What is the complete diagnosis?
(2 marks)
...................................................................................................
3. State Appropriate (A) or Inappropriate (I) for each of the following steps in the management at this stage
(8 marks):
a. Obtain radiographs of the right knee and refer to orthopaedic surgery
( )
b. Ultrasound/MRI of the right knee and refer to interventional radiology
( )
c. Aspirate the right knee and send fluid for gram stain and culture
( )
d. Aspirate the largest skin lesion and send fluid for gram stain and culture
( )
e. Urethral swab for gonorrhoea and Chlamydia-PCR
( )
f. Midstream urine for gram stain and culture
( )
g Blood culture and start antibiotics immediately
( )
h. Check serum uric acid levels and start colchicine and/or nonsteroidal anti-inflammatory drugs
( )
i. Check rheumatoid factor and consider adjuvant low-dose prednisolone
( )
j. Notify the Ministry of Health
( )
4. What important advice would you give this patient?
(2 marks)
a. ...............................................................................................
b. ...............................................................................................
Question 1.2
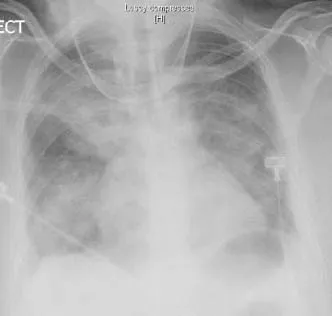
A 42-year-old female with Down syndrome presented with shortness of breath for a week, associated with spiking fever and poor oral intake. Her mother noted occasional wheezing and lips turning “blue.” Clinically, her pulse rate was 110/min, blood pressure 95/70 mmHg and pulse oximetry 90% on room air. She had coarse crepitations over the lung bases.
1. Describe the abnormalities seen on the chest X-ray.
(4 marks)
...................................................................................................
...................................................................................................
2. What is the complete clinical diagnosis?
(2 marks)
...................................................................................................
3. Where would you propose to send this patient to from the Emergency Department?
(1 mark)
a. General ward
b. Isolation ward
c. High-dependency unit
d. Follow-up at general practitioner clinic in two days
e. Admission not necessary at this stage, but early outpatient review needed
( )
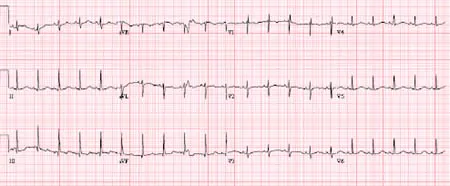
4. State two gross abnormalities in her electrocardiogram.
(2 marks)
a. ...............................................................................................
b. ...............................................................................................
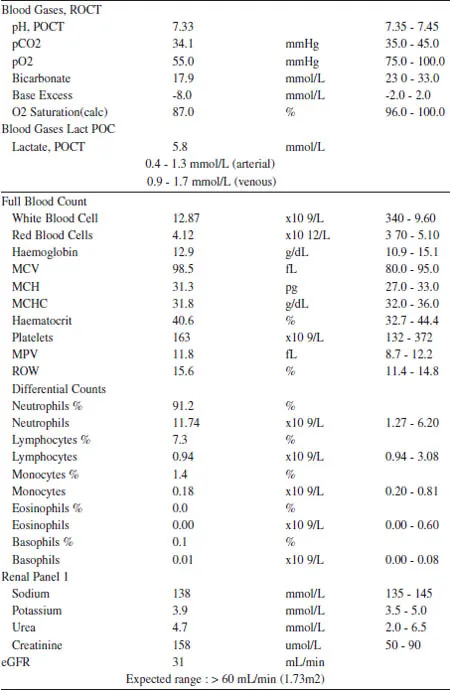
Below are her initial laboratory test results:
5A. What abnormalities are seen on her arterial blood gas result?
(2 marks)
...................................................................................................
...................................................................................................
5B. Comment on her full blood count and renal function tests.
(4 marks)
...................................................................................................
...................................................................................................
...................................................................................................
Her fever lysed after two days of appropriate therapy. However, she remained on 50% non-rebreather mask. This is ...