![]()
Chapter 1
Resuscitation Service: An Overview
Introduction
Every hospital has a duty of care to ensure that an effective and safe resuscitation service is provided for its patients. The satisfactory performance of the resuscitation service has wide-ranging implications in terms of resuscitation equipment, resuscitation training, standards of care, clinical governance, risk management and clinical audit (Jevon, 2002; Royal College of Anaesthetists et al., 2008). Standards for resuscitation and resuscitation training have been published (Royal College of Anaesthetists et al., 2008).
The aim of this chapter is to provide an overview to the resuscitation service in the hospital setting.
Learning outcomes
At the end of the chapter the reader will be able to:
- Discuss the concept of the chain of survival
- Summarise Cardiopulmonary Resuscitation: Standards for Clinical Practice and Training
- Discuss the key recommendations in the joint statement
- Discuss the principles of safer handling during cardiopulmonary resuscitation (CPR)
Concept of the chain of survival
Survival from cardiac arrest relies on a sequence of time-sensitive interventions (Nolan et al., 2006). The concept of the original chain of survival emphasises that each time-sensitive intervention must be optimised in order to maximise the chance of survival: a chain is only as strong as its weakest link (Cummins et al., 1991).
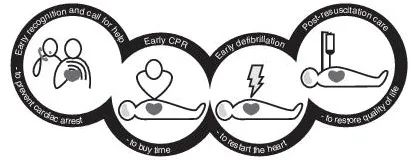
Fig. 1.1 Chain of survival. Reproduced with permission from Laerdal Medical Ltd, Orpington, Kent, UK.
The chain of survival was revised in 2005 (Figure 1.1) to stress the importance of recognising critical illness and/or angina and preventing cardiac arrest (both in and out of hospital) and post-resuscitation care (Nolan, 2005):
- Early recognition and call for help to prevent cardiac arrest: this link stresses the importance of recognising patients at risk of cardiac arrest, calling for help and providing effective treatment to hopefully prevent cardiac arrest; up to 80% of patients sustaining an in-hospital cardiac arrest have displayed signs of deterioration prior to collapse (Nolan et al., 2006); most patients sustaining an out-of-hospital cardiac arrest also display warning symptoms for a significant duration before the event (Muller et al., 2006)
- Early CPR to buy time and early defibrillation to restart the heart: the two central links in the chain stress the importance of linking CPR and defibrillation as essential components of early resuscitation in an attempt to restore life
- Post-resuscitation care to restore quality of life: the priority is to preserve cerebral and myocardial function, to restore quality of life and indicates the potential benefit that may be provided by therapeutic hypothermia
(Nolan et al., 2006)
Cardiopulmonary Resuscitation: Standards for Clinical Practice and Training
Cardiopulmonary Resuscitation: Standards for Clinical Practice and Training (Royal College of Anaesthetists et al., 2008) is a joint statement from the Royal College of Anaesthetists, Royal College of Physicians of London, Intensive Care Society and Resuscitation Council (UK). It has been endorsed by a number of national bodies, including the Royal College of Nursing and builds on previous reports and guidelines including those from the Royal College of Physicians and Resuscitation Council (UK) (Royal College of Anaesthetists et al., 2008).
The joint statement makes a number of recommendations relating to:
- The resuscitation committee
- The resuscitation officer
- Resuscitation training
- Prevention of cardiopulmonary arrest
- The resuscitation team
- Resuscitation in children, pregnancy and trauma
- Resuscitation equipment
- Decisions relating to CPR
- Patient transfer and post-resuscitation care
- Audit and reporting standards
- Research
Key recommendations in the joint statement
Resuscitation committee
Each hospital should have a resuscitation committee that meets on a regular basis and is responsible for implementing operational policies relating to resuscitation practice and training. The chairperson should be a senior clinician who is actively involved in resuscitation. Membership of the committee should include:
- A physician
- A senior resuscitation officer
- An anaesthetist/intensivist
- A senior manager
- Representatives from appropriate departments, for example, accident and emergency (A&E), paediatrics, based on local needs
Responsibilities of the resuscitation committee include:
- Advising on the composition and role of the resuscitation team
- Ensuring that resuscitation equipment and resuscitation drugs are available
- Ensuring the adequate provision of resuscitation training
- Ensuring that Resuscitation Council (UK) guidelines and standards for resuscitation are followed
- Updating resuscitation and anaphylaxis policies
- Recording and reporting clinical incidents related to resuscitation
- Auditing resuscitation attempts and do not attempt resuscitation (DNAR) orders
Resuscitation officer
Each hospital should have a resuscitation officer responsible for resuscitation training, ideally one for every 750 clinical staff. The resuscitation officer should possess a current Resuscitation Council (UK) advanced life support (ALS) certificate and should ideally be a Resuscitation Council (UK) ALS instructor. Adequate training facilities, training equipment and secretarial support should be provided. Responsibilities of the resuscitation officer include:
- Implementing Resuscitation Council (UK) guidelines and standards in resuscitation
- Providing adequate resuscitation training for relevant hospital personnel
- Ensuring there are systems in place for checking and maintaining resuscitation equipment
- Auditing resuscitation attempts using the current Utstein template
- Attending resuscitation attempts and providing feedback to team members
- Coordinating participation in resuscitation-related trials
- Keeping abreast of current resuscitation guidelines
Resuscitation training
Clinical staff should receive regular (at least annual) resuscitation training appropriate to their level and expected clinical responsibilities. It should also be incorporated in the induction programme for new staff. The training should include the recognition and effective treatment of critical illness and providing effective treatment to prevent cardiopulmonary arrest. Some staff, e.g. members of the cardiac arrest team, will require appropriate advanced resuscitation training, e.g. Resuscitation Council (UK) Advanced Life Support (ALS) Course (see Chapter 17).
Extended nursing roles in resuscitation should be encouraged – for example, airway adjuncts, intravenous cannulation and administration of specific emergency drugs, electrocardiogram (ECG) interpretation and defibrillation.
The resuscitation officer is responsible for organising and coordinating the training; a cascade system of training may be needed to meet training demands, particularly in basic life support. Help should be sought from other medical and nursing specialities to provide specific training, such as in neonatal resuscitation.
See Chapter 17 for more detailed information on resuscitation training.
Prevention of cardiopulmonary arrest
Systems should be in place to identify patients who are critically ill and therefore at risk of cardiopulmonary arrest (Royal College of Anaesthetists et al., 2008). Every hospital should have an early warning scoring system in place to identify these patients; adverse clinical indicators or scores should elicit a response to alert expert help, e.g. critical care outreach service, medical emergency team (National Institute for Health and Clinical Excellence (NICE), 2007).
Each healthcare organisation should have a patient’s observation chart that facilitates the regular measurement and recording of early warning scores; there should be a clear and specific policy that requires a clinical response to ‘calling criteria’ or early warning systems (‘track and trigger’), including the specific responsibilities of senior medical and nursing staff (Royal College of Anaesthetists et al., 2008). For further information see Chapter 3.
The resuscitation team
Every hospital should have a resuscitation team. Ideally, this should include a minimum of two doctors who are trained in advanced life support. The resuscitation committee should advise on the composition of the cardiac arrest team, but overall the team should be able to perform:
- Airway management (including tracheal intubation)
- Intravenous cannulation (including central venous access)
- Defibrillation (advisory and manual) and electrical cardioversion
- Drug administration
- Advanced techniques, e.g. external cardiac pacing and pericardiocentesis
- Appropriate skills for effective post-resuscitation care
The resuscitation team should have a team leader (usually a doctor), whose responsibilities include:
- Directing and coordinating the resuscitation attempt
- Ensuring the safety of the patient and the team
- Terminating the resuscitation attempt when indicated
- Communicating with the patient’s relatives and other healthcare professionals
- Documenting the resuscitation attempt (including audit forms)
The resuscitation team should be alerted within 30 seconds of dialing 2222 (recommended telephone number for contacting switchboard following an in-hospital cardiac arrest) (National Safety Patient Agency (NSPA), 2004). The system should be tested on a daily basis.
Resuscitation in children, pregnancy and trauma
Children: ideally, there should be a separate paediatric resuscitation team, with the team leader having expertise and training in paediatric resuscitation. All staff who are involved with paediatric resuscitation should be encouraged to attend national paediatric courses, e.g. European Paediatric Advanced Life Support (PALS), Advanced Paediatric Life Support (APLS) and Newborn Life Support (NLS).
Pregnancy: an obstetrician and a neonatologist should be involved at an early stage; minimising vascular compression by the gravid u...